The Christopher Ellington Story – A Chiari Warrior’s Journey [Updated]
My introduction to Chiari malformation I (CM1) begins in 1994. I had been married about 7 months and we had just celebrated our first Christmas together as newlyweds. Shortly after the new year, I developed a bad headache that eventually evolved into losing my eyesight in one eye. I went to the eye doctor, who immediately sent me to the hospital. I was diagnosed with Pseudotumor Cerebri and Papilledema, which are known to often accompany Chiari (co-morbid conditions). At the time, we were told that it was likely due to a virus. I had five failed lumbar punctures and finally a successful sixth in radiology, was given Diamox, and the problems went away. Nothing was ever said about Chiari or an abnormal MRI. I also had no idea that I could or should get a copy of the MRI from the hospital, so I could keep my own records. I wasn’t even given any reason on why it might be necessary. I trusted my doctors and they helped resolve the problem with my sight. Little did I realize that it was only the beginning and I was in for the fight of my life!
From 1994 until 2005, I had few further significant issues. I continued to have headaches which I treated with Excedrin and ringing in my ears (tinnitus), which was generally attributed to the aspirin in the Excedrin and sinus issues. In January of 2005, I started having jaw pain. I saw a number of dentists and doctors who couldn’t figure out the problem. I eventually ended up seeing a doctor specializing in pain management who indicated he thought it was Trigeminal Neuralgia (which is another co-morbid disorder of Chiari, but its connection wasn’t made known to us). I was sent to a neurologist, who pointed out I had a 2cm (20mm) herniation, which he said wasn’t enough to worry about, but it was a Chiari malformation. Again, he was the doctor, so we just trusted that it wasn’t something to worry about. The pain worsened: it started lasting for longer periods of time and increased in both intensity and frequency, so I went to the ER on the advice of the neurologist for pain relief. When I arrived, the neurosurgical group that I had an appointment with had left word for me to go to their office, so I could see them. Since my appointment wasn’t for another several weeks, we were thrilled to get in so fast. We were also told I had Trigeminal Neuralgia and that Chiari wasn’t related and that Chiari couldn’t kill you; although they informed me that I would need surgery. I was scheduled for a decompression surgery almost immediately and thought I was cured. The neurosurgeons indicated that a 2cm (20mm) herniation was quite significant and that I was “in good hands.” The decompression was somewhat successful in that it resolved some of my symptoms, but the relief was short lived.
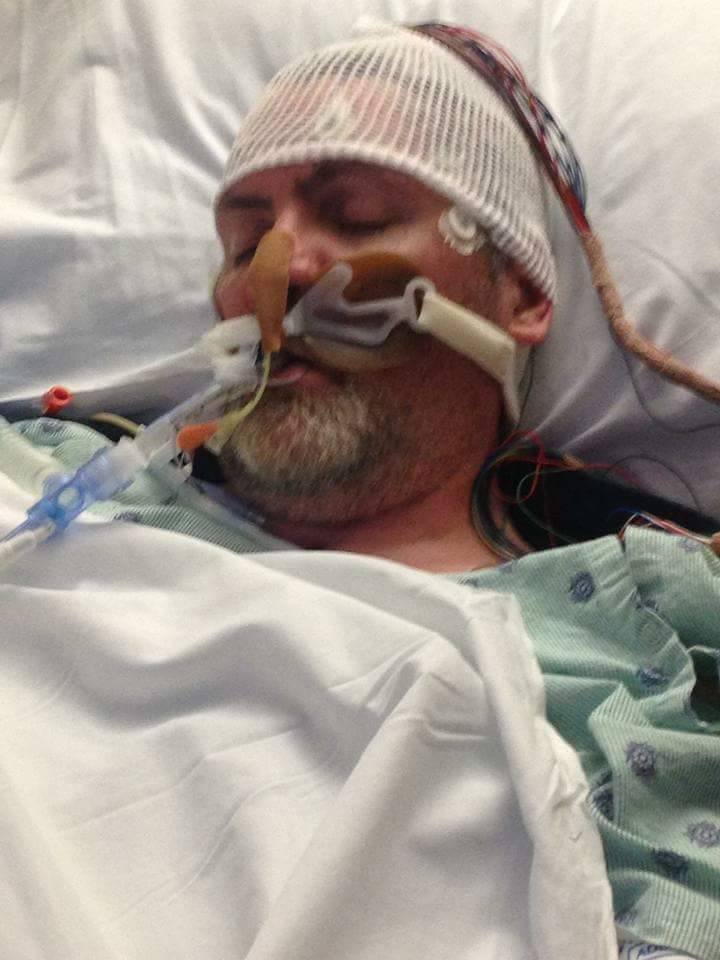
I stopped taking the Gabapentin for Trigeminal Neuralgia but began having trouble with balance issues and nobody was sure why. I was told that the Chiari had nothing to do with any of this and that I was “just lucky” that all my conditions were minor. My surgeon considered Microvascular Decompression (MVD), but said I was “too tight” and the surgery wouldn’t be a good idea. In January 2007 and November 2007, I had rhizotomies performed to deaden the nerve. The rhizotomy only worked for about six months before the pain returned. I had a repeat rhizotomy in November 2007 and that has been successful to date. I was still having a lot of symptoms (that I now know to be Chiari symptoms) but they continued to assume them to be due to the Pseudotumor Cerebri, even though I didn’t have my pressure checked or any sign of a papilledema. In June 2008, I had a Ventriculoperitoneal (VP) shunt put in. It was ligated (tied off) in July 2010 since I had lost weight and the symptoms had switched from what was presumed to be high pressure to low pressure symptoms. Due to my new low-pressure symptoms, they tried several blood patches in an attempt to repair what was assumed to be a leak, even though it was never found on any of the testing. Initially, the blood patches worked well, but over time the blood patches were less effective, and I started getting headaches again. Eventually, the doctors gave up on blood patches as they weren’t helping the headaches and finally, I stopped getting headaches (which we later found out wasn’t uncommon for those who have had long-term CSF leaks.
Despite my lack of headaches, I started having neurodegenerative problems: trouble maintaining consciousness, hypersomnolence, severe balance problems, bouts with confusion and cognitive changes. My neurologist became convinced that I needed a second decompression. He discussed my case with my neurosurgeon who initially didn’t think that another decompression would help. He was convinced to perform the surgery and I had the decompression in January 2012. The decompression was very successful for 23 days. After that, I declined rapidly. Over the next year, I developed multiple lung infections, which they presumed to be from my history as a smoker, but in reality, it was due to dysphagia. In January 2013, I was admitted to the hospital for yet another lung infection and by May, I was given a feeding tube. My wife was brought into a meeting with my neurologist where he said I needed to go to a nursing home and that my death could be imminent. I went to the nursing home and did better than they expected. Instead of dying at the nursing home, I improved and was released to go home a month later. I continued to improve enough to have the feeding tube removed that July.
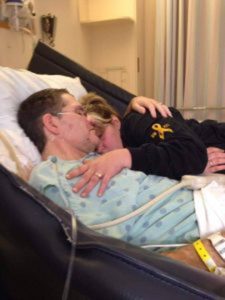
Once home, my condition continued to decline. My wife continued researching and we decided to go and see a Chiari specialist since her research indicated it was the only real way to proceed, especially with a difficult case. In June 2014, we met with one such expert who was able to explain why the first two decompressions failed. Ehlers-Danlos Syndrome and Craniocervical Instability were two of the missing pieces to my puzzle. It was an eye-opening experience and finally, my issues made sense. We discussed several options for surgery, and eventually settled on a date, October 30, 2014. I had my third decompression and this time, a spinal fusion. It was a wild success! Many of my symptoms were resolved immediately. While it was not a cure, it certainly helped me substantially in restoring many functions and my quality of life.
However, in September 2015, I went into a coma while hospitalized for a reduced state of awareness (which coincided with weaning off the Decadron) and the local doctors said it was another failed decompression. In October 2015, I had yet another MRI. While going over the radiologist report, my wife noticed something none of my doctors mentioned, it stated that I had severe Intracranial Hypotension. My wife sent my MRI images to a leak expert and my NY neurosurgeon for further assessment.
In January 2016, I was in another hospital across the country having imaging for the known CSF leak. After the testing was done, a leak was found in my lumbar spine and a location they felt was suspicious on my thoracic spine (where I had old stress fractures and incredibly thin dura, believed to have been causing leaks). There were also bone fragments next to the fractures, so the doctor double reinforced my spine in that area and performed a dural reduction surgery in parts of my thoracic and lumbar spine. I got better until August 2016, when I started experiencing symptoms of a CSF leak. Upon consultation, we decided a blood patch would be the place to start and it resolved my symptoms quickly. As of August 2018, the blood patch has continued to keep me from leaking and no leak symptoms have occurred. While I’m going to be at risk for leaks, and likely leak periodically due to Ehlers-Danlos Syndrome, I will take the results I’ve seen thus far. It’s also interesting to note that while I’ve had a number of unsuccessful patches, this time the post-patch recovery protocol was different in that I laid flat for 2 hours post patch, then 3 days lying flat except to go to the bathroom and eat. I’m convinced that this protocol helped immensely, as the weight of the CSF Is much greater when upright thus increasing the chance of a leak. Also, a blood patch doesn’t end the leak repair, it merely starts it. Once the clotting effect has finished, the next stage occurs, which includes tissue growth to repair the opening. With Ehlers-Danlos Syndrome, this process is often diminished and requires longer than the normal recovery time, which is why I believe many of us have had failed patches.

I am still continuing to heal, and likely will never be returned to my old self. I have been discharged from physical therapy as of December 2017, however I still exercise every day for at least an hour. I know that this is a key part of my healing; there have been a few occasions when I was unable to do my exercises for a few days I notice difficulty in doing my daily activities. In addition, I will not likely be able to work as a paid employee ever again, however, I have been able to provide some help to a variety of people. I enjoy helping others and this works well as if I have a less than optimal day, I can just let anyone who needs my help know that I won’t be available to help them.
My recovery hasn’t been without trouble, as I returned to the hospital once, in the spring of 2018, for what was presumed to be a gall bladder problem. Since I’ve suffered issues with kidney stones, it’s not surprising to me that I have a lot of gall stones. I suspect it has to do with some of the gastrointestinal issues that hEDS brings, but there is nothing definitive. After 2 days of pretty significant pain, the pain subsided and nothing more came of it.
Overall, there have been a number of positive outcomes and I wouldn’t change the decision to have my third decompression & fusion. This has granted me the ability to lead a life, which while not “normal,” is fulfilling.
I am not, and never will be, completely healed. Many of my symptoms have resolved to the point where I can tolerate them and at times, don’t even notice them. While there is no cure for Chiari or the Ehlers-Danlos Syndrome causing it all, there is more healing possible. They are difficult disorders for many reasons and one of the biggest issues is the way it presents itself; for each person, it can be entirely different, making the diagnosis very difficult. I will always have to be monitored for leaks each time the symptoms present themselves, but for now, I find myself thankful to be alive and so very lucky to have the support I do, especially from my wife, my hero!
*Updated August 2018
3 comments
Reply
You must be logged in to post a comment.

What a harrowing story. But it shows how much our loved ones advocating for us can do, and how important it is to research and understand these conditions and get to a real specialist!
Heartbreaking. Thank you for sharing your love my journey with us.
This young man is quite the warrior. This story just goes to show the importance of seeing a true chiari specialist. Too often we trust doctors who say they are familiar with chiari, but being familiar is not enough. We have to be vigilant about our health and see doctors who are known chiari specialists if we are to be under the best care.